At the time I am writing this, my home city (New York City) has become the epicenter of the coronavirus disease (COVID-19) pandemic in the United States. [1] Per the advice of health experts, I’m staying at home as much as possible, washing my hands regularly, and practicing social distancing when outdoors (I get outside daily for socially distant exercise and sun), along with eating healthy, getting adequate sleep, and minimizing stressors.
I am also taking proactive measures by tracking several key vital signs that have been shown to correlate with many COVID-19 symptoms. Many people have been asking me about which vital signs I am closely monitoring, which I am happy to share.
COVID-19 Symptoms and Risk Factors
Let’s start by looking at what the CDC (Centers for Disease Control and Prevention in the US) has identified to be leading COVID-19 risk factors, symptoms, and complications: [2]
Risk Factors: age, serious underlying medical conditions (e.g. heart or lung disease, diabetes, lung disease, etc).
Symptoms: fever, cough, shortness of breath or difficulty breathing, chills, repeated shaking with chills, muscle pain, headache, sore throat, new loss of taste or smell.
Complications: pneumonia, Acute respiratory distress syndrome (ARDS), kidney failure.
1. Body Temperature
One common COVID-19 symptom is a low-grade fever that gradually increases in temperature. [3]
That is because developing an elevated body temperature is common when fighting off illness or infection. For example, I caught a flu (pre-coronavirus) just before the new year. My Ōura data showed that my skin temperature started increasing just prior to the moment I had to spend 1.5 days lying on the couch fighting off shivers and fatigue:

Tracking Body Temperature
In addition to my Ōura data, I also take body temperature readings at the same time each day to monitor for any increasing trends versus my baseline resting heart rate. I have been using a Kinsa smart thermometer as well as a traditional analog mercury-free basal thermometer (any decent thermometer will do).
Note: Please keep in mind that elevated body temperature could be due to other factors such as overconsumption of alcohol.

2. Resting Heart Rate
A higher resting heart rate (the number of beats per minute while sitting or sleeping) can be another sign that the body’s immune system is ramping up for a fight. [4]
Tracking Resting Heart Rate
All of the major wearables today track resting heart rate. What is important is to understand your personal baseline resting heart rate. Going back to my flu episode, you can see that my resting heart rate jumped up by more than 20 beats per minute:

Note: Women should pay close attention to menstrual cycle in the context of resting heart rate, as resting heart rate may change just prior to menstruation and ovulation.

3. Blood Oxygen Saturation (SpO2)
The most worrisome complication related to COVID-19 is a drop in oxygen levels in the body, where the compromised lungs have a harder time getting oxygen into the blood and to important organs [4] (this is why there is a huge demand for ventilators).
Tracking Blood Oxygen Saturation (SpO2)
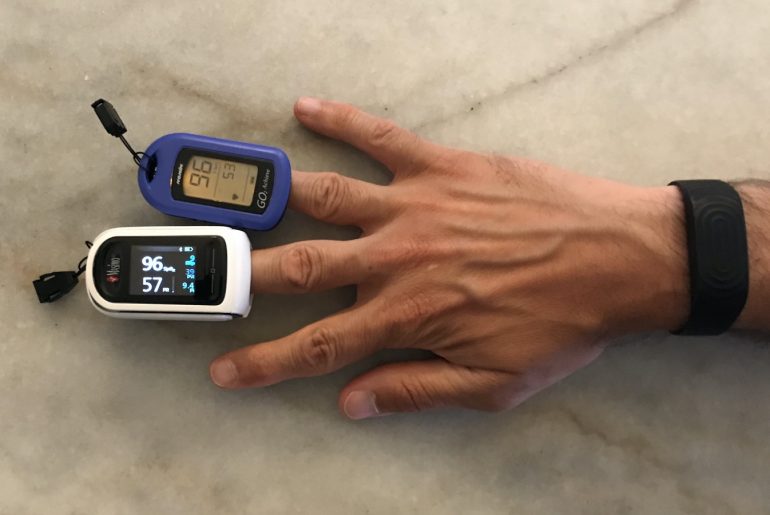
A device called a finger pulse oximeter is used to measure peripheral capillary oxygen saturation, or SpO2. SpO2 is the percentage of hemoglobin in the blood that is oxygen-saturated. A healthy adult will usually see readings in the range of 95-100 percent, and levels below 90 percent are considered dangerously low (hypoxemia).
Most finger pulse oximeters are inexpensive and can be purchased at any pharmacy or online (I use this higher-end bluetooth-enabled model from Masimo for other workouts and breathwork). Simply place the pulse oximeter over one of your fingers and it will provide a reading in a few seconds. Again, it’s all about understanding one’s baseline and paying attention to any drops in SpO2 levels.
Biostrap makes another great general fitness/sleep tracker that can monitor SpO2 readings overnight as well.
Note: Smokers may observe artificially elevated readings due to the fact that carbon monoxide (CO) may bind to hemoglobin in the blood — pulse oximeters cannot differentiate oxygen- from carbon monoxide–bound hemoglobin. [5]

4. Blood Pressure
Hypertension is not only a key risk factor for getting COVID-19, but research is showing that those with it may be more likely to have worse symptoms and have a higher mortality rate. [6]
Tracking Blood Pressure
Home blood pressure monitors can also be purchased at any pharmacy, or online retailer. I use an older version of this device from Omron. A cuff is placed around the arm, which then inflates, then slowly delates. Blood pressure readings will appear in the format like “125/75”, where the top number is called systolic blood pressure (indicates how much pressure your blood is exerting against your artery walls when the heart beats), and the bottom number is called diastolic blood pressure (indicates how much pressure your blood is exerting against your artery walls while the heart is resting between beats).
Note: You’ll want to take readings away from any caffeine, exercise, or large meals as they may affect you readings. Follow instructions about optimal sitting posture to ensure accurate readings. As there can be some acute variability, I usually take two consecutive readings, then average the numbers.
Coronavirus-related Symptom Trackers and Research Studies
A number of organizations and companies are putting together tools and studies for using data from wearable devices to monitor for flu and COVID-19 to understand which factors most correlate with and/or predict illness:
Quantified Flu (Open Humans) – https://quantifiedflu.org/
UCSF TemPredict Study – https://ouraring.com/ucsf-tempredict-study
Kinsa Health Weather Map – https://healthweather.us/
Heads Up Health COVID-19 Dashboard – https://www.headsuphealth.com/covid19
COVID-19 Immune – https://covid19immune.com/
References
[1] https://www.nytimes.com/2020/03/22/nyregion/Coronavirus-new-York-epicenter.html
[2] https://www.cdc.gov/coronavirus/2019-ncov/symptoms-testing/symptoms.html
[3] https://www.webmd.com/cold-and-flu/news/20200117/could-your-fitbit-help-detect-the-flu
[4] https://www.npr.org/sections/goatsandsoda/2020/02/14/805289669/how-covid-19-kills-the-new-coronavirus-disease-can-take-a-deadly-turn
[5] https://www.ncbi.nlm.nih.gov/pubmed/?term=buckley+pulse+oximetry+gap
[6] https://www.webmd.com/lung/coronavirus-high-blood-pressure